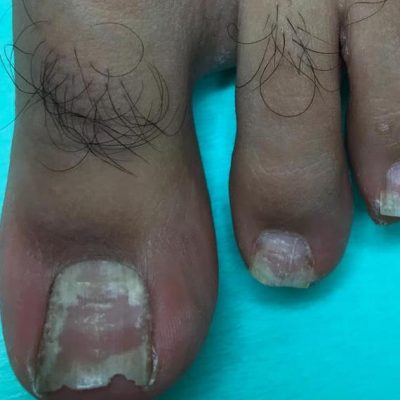
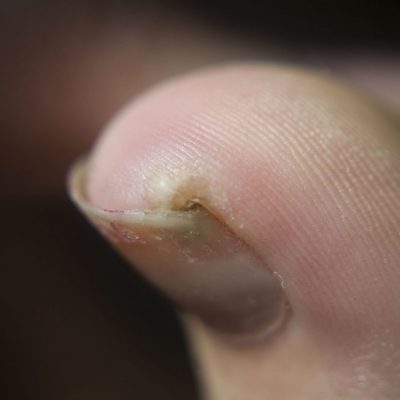
Corns and Callous Treatment
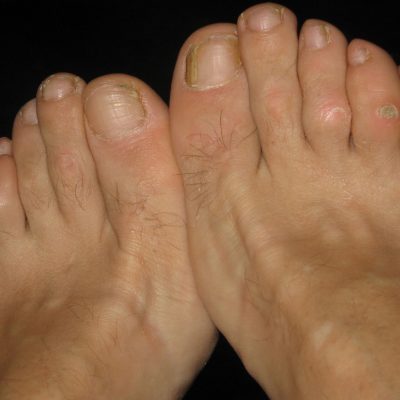
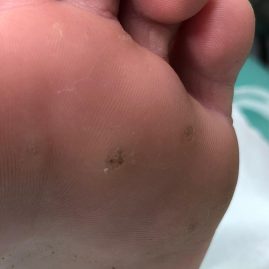
Callus can form on areas of the feet where there may be excessive pressure or friction during activity or when wearing certain types of footwear. There are other factors which may also contribute to callus formation.
Osteoarthritis and rheumatoid arthritis can change the shape of joints and there is often also associated swelling around the joints in these conditions. Inflammation and swelling can become painful which can in turn have an impact upon mobility, the formation of callus will undoubtedly add to the discomfort or pain.
If these factors remain continuous there may be formation of corns which apply pressure to the deeper layers of the skin causing more acute pain further affecting mobility.
In those whose mobility is already an issue, these added problems can certainly further destabilise gait.
However it is not only these groups of people who will suffer discomfort, pain and destabilisation from corns and callus formation. They can hamper the performance of runners, footballers and many other sporting and recreational activities .
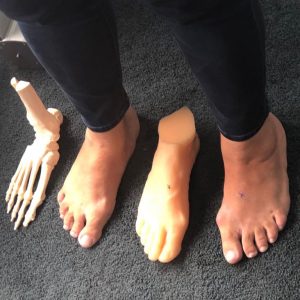
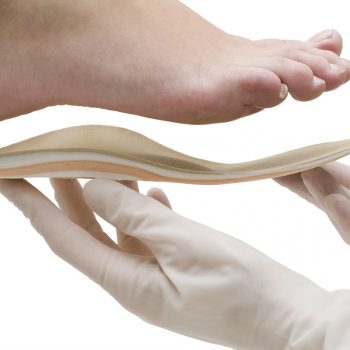
Biomechanics can help these conditions and therefore the varied groups of people. The Podiatrist will carry out a thorough and systematic assessment looking at alignment, muscle flexibility, joint range of motion, gait and more in order to gain a deeper insight into the possible cause of gait type and ultimately the formation of callus and corns. The information gained can then be used to determine what type of exercise regime might be beneficial and also what type of orthotics will help to improve the way that the feet work.
Contact us to book your biomechanics assessment now and take control of your foot issues.